by Valiant | Oct 14, 2018 | Addiction treatment, teen drug use
While you can’t experience it for yourself unless you decide to go that route, you can sometimes find someone who has overcome their addiction and is willing to give you a first-hand glimpse into what exactly the life of an addict is like. Recently on CBC News,...

by Valiant | Sep 27, 2018 | Addiction treatment
Every year, the Substance Abuse and Mental Health Services Administration (SAMHSA) sponsors Recovery Month. It is designed to increase understanding and awareness of both mental and substance use disorders. Additionally, it is to celebrate those who have recovered...
by Valiant | Jul 24, 2017 | Addiction treatment
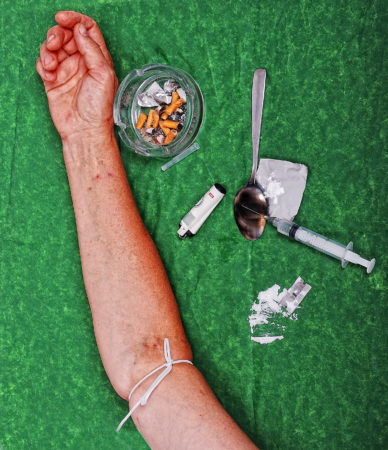
When it comes to addiction, one of the things we have to be realistic about is the possibility of overdosing. This is a very real concern especially with the overdose emergency of opioids going on today. In the community, there are Naloxone kits available to you and...
by Valiant | Aug 26, 2016 | Addiction treatment, Alcohol abuse, Drug abuse
Before treatment, it is common for friends and family to enable the addict, or to try and protect them from the consequences of their alcohol or drug abuse. Sometimes loved ones do not address the substance abuse because they fear pushing the person away or alienating...
by Valiant | Aug 22, 2016 | Addiction treatment, Alcohol abuse
Denial by both alcoholics, their friends, and family is one of the most powerful processes that keep the cycle of addiction going. It hides the damage and the importance the issue in ways that eliminate any chance of recovery. Facing facts with simple questions is a...
by Valiant | Aug 19, 2016 | Addiction treatment, Drug abuse, Prescription drug abuse
Investigators at Massachusetts General Hospital have determined that stimulant medication misuse increases the risk of conduct problems, substance abuse, and ADHD among college students when compared to peers who did not misuse stimulant medication. The investigators...




